Pharmacogenetics DNA test best use
Dr.M.Raszek
Personalized medicine – getting the right medication to the right person at the right time
Traditionally medicines have been developed to target entire populations. However, it has been understood for a long time that patient’s individual biological influences can dramatically shift drug effectiveness in comparison to just the population average. For this reason medication efficacy can actually be astonishingly low for any given person - far lower than people probably realize.
It is not that these medications are not good. They can be incredibly good if they are correctly targeted to the right people. Before pharmacogenetics we simply did not have a really good means to be able to properly cross reference patients and drugs, and as a result we take a somewhat random chance if the medication will be effective or not when we take a drug.
However, now we actually have the means to start probing this information of how to properly match medications to an individual. It is based on a person’s genetics especially the specific mutations in a person’s DNA code that can result in differences in how we biologically react to a specific medication. This is referred to as pharmacogenetics (PGx for short).
Pharmacogenetic testing provides doctors with a guideline on how to prescribe the optimal drug with the optimal dosage to a patient based on their individual unique genetic map. We previously touched on this topic when we analyzed drugs used in childbirth for pharmacogenetic associations. Drugs with pharmacogenetic information have been approved by regulatory agencies around the world. For those medications with approved pharmacogenetic information, the drug labels now actually list the pharmacogenetic information for patients to research for themselves. In some cases this is merely a recommendation from the regulatory agency. In others it is even required for the medication to be prescribed.
There are many pharmacogenetic DNA tests out there with a wide range in quality, so do not just go out and buy the first one you encounter. Typically these tests will only look for very specific mutations within the DNA of select genes (this is referred to as genotyping). This is a very cheap and rapid analysis, and the reason why some pharmacogenetic tests are fairly low cost. However, for clinical use the type of DNA tests that provide a more thorough investigation is preferred. These tests also assess if any of the genes of interest might have been duplicated. This is referred to as copy number variation and you can appreciate that if you duplicate a gene which will result in more enzymes processing a drug, then that could seriously affect how the drug is then handled by the body.
The more expensive tests also will employ a team of experts to manually analyze results whereas cheaper tests are all automated with no or limited human oversight. Finally, it is the resources that are used by the testing company that can also influence the cost, such as which databases are used to assess the genetic impact on medication, or the type of programming developed to test for complicated multiple variables such as interaction of multiple genes on the same drug, or more rarely (and this is especially valuable), how different drug combinations could be affecting overall performance. This interplay of factors can be so complex to navigate through, that the most sophisticated tests will actually employ complex artificial intelligence and machine learning approaches for the most advanced results.
In fact, the poor quality of some of the commercially available pharmacogenetic DNA tests has prompted the FDA to start going after these companies. The only problem is that the witch hunt has extended to even highly reputable companies for supporting genetic testing for drugs that are not FDA approved for pharmacogenetic testing. This is very unfortunate as the FDA is not expected to be the authority on pharmacogenetics at all. There are other more qualified organizations and one of the best is the ‘Pharmacogenomics Knowledgebase’ (PharmGKB), an NIH-funded database of pharmacogenetic information. There are many other drug-gene associations that are very well established which have yet not been “approved” by FDA.
How does pharmacogenetics work?
Essentially the enhanced efficacy of medication use is driven by two aspects:
- Determining the correct dose of medication to be used for a patient
- Determining safety of medication prior to prescription
For further details on this, and to learn who can benefit most from PGx testing, please check out the video below. Pharmacogenetic DNA test’s best usage is detailed in the video.
When it comes to determining dosing, this is primarily driven by determining how the enzymes (your tiny molecular robots inside your body) actually break down the drug based on the mutations that are uncovered in your DNA (DNA mutations determine how these molecular robots are built).
For example, cytochrome P450 (CYP450) enzymes are a super family of enzymes responsible for the metabolism of the vast majority of drugs. Mutations in these enzymes can affect their function and therefore the extent to which they can process a drug. It is this information that is assembled together to label a patient within a specific category of drug metabolism ability.
Poor metabolizers are those patients that have less active or inactive enzymes. These individuals run the risk of experiencing a drug overdose or an increase in toxicity because a normal drug dose is applied to them (based on an average dose curve of normal metabolizers). Their drug dose would have to be reduced instead.
Conversely, ultra-rapid metabolizers might have multiple copies of a particular gene responsible for drug break down and in that case the drug might be metabolized so rapidly that such patients might not get any efficacy from the drug. Their drug dose might have to be increased.
The exact opposite effects would be expected for prodrug compounds (drugs that need to be broken down first in order to release the active compound, for example clopidogrel or codeine, both of which have PGx associations). Thus prodrugs can be non-effective in poor metabolizers, while in ultra-rapid metabolizers the active compounds could build up to such high levels as to produce toxic side effects.
In a nutshell, a pharmacogenetic testing’s purpose is to help with the more effective use of drugs by improved dosages and reduced toxic side effects and by overall improved treatment we would expect this to lead to faster patient recovery. Now, let us take a look at what might be the impact of the misuse of drugs leading to toxic side effects.
Toxic drug side effects – what are your odds?
Drug toxic side effects (referred to in scientific literature as adverse drug reactions so as not to sound so provocative) can account for up to 7% of all hospital admissions, up to 20% of re-admissions and approximately 0.3% of all hospital deaths according to one of the most authoritative landmark studies on this subject. This might not sound like much but this is equivalent to over a hundred thousand deaths in the US, easily making it into the top ten leading causes of death. This is not frequently reported in cited causes of death, so the public is largely unaware of these risks associated with medicating. It is surprising because the Center for Disease Control and Prevention reporting on the leading causes of death does report deaths due to accidental injuries in their top ten list, so there is no specific reason why drug misuse should not be included as well.
For a deep dive into actual clinical trials, we wanted to share one interesting Italian study. This study was specifically for internal medicine patients, or diseases affecting patients’ inner organs. This especially represents the older population of the society, with 75.4% of the studied patients being over the age of 65 years. This is perhaps good to examine because this older population also showed which health problems are especially susceptible to unwanted drugs reactions - a valuable warning that could be extended to younger patients. However, cancers and mental disorders will be under-reported because these patients can be treated in different departments of assessed hospitals.
While this clearly is not representative of the world, this study helps to answer many questions at once, so we can simply use it as a ballpark just to see what can be expected. Whichever age bracket you find yourself in, let’s see if any of the below bits of information might apply to you in terms of the risk of experiencing drug side effects.
If any of it does, and your medication has a pharmacogenetic link, then you can evaluate if the pharmacogenetic DNA test is worth your investment or not. Luckily, pharmacogenetic tests are actually on the cheaper side of the DNA tests involved in a clinical setting.
Health issues most frequently linked with drugs toxic side effects
A picture is worth a thousand words so let’s pop out some graphs and let the visuals speak for themselves.
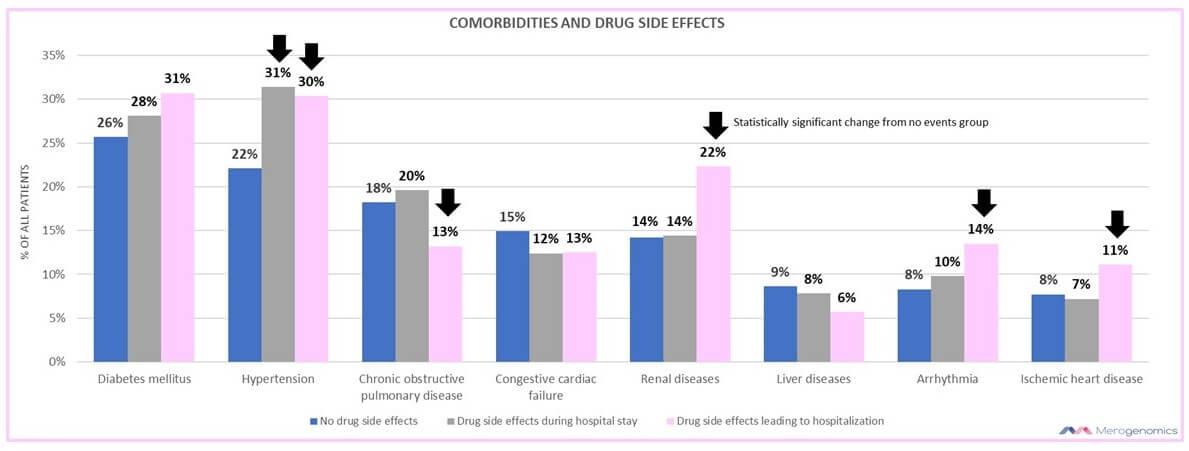
As you can see, your existing health issues that require medical attention (comorbidities) are very unlikely to be an influencing factor for experiencing drug toxic side effects once you are in a hospital setting. Only hypertension poses an increased risk. This is really an interesting way to observe how good our healthcare staff is in managing patients in a very challenging environment.
However, people who are left to treat themselves and who end up being hospitalized due to drug adverse reactions are a different story, and now many comorbidities appear to have a negative influence (diabetes also just missed the statistical cut off). If you are treating yourself for any of these health issues, it might be worth to check if your medications have any genetic association.
Conditions with the highest chance of experiencing drug toxic side effects
The types of disorders that are most frequently associated with drug toxic side effects also warrant consideration in the use of pharmacogenetic testing to try to mitigate these adverse events.
Conditions most often encountering drug toxic side effects leading to hospitalization were gastrointestinal disorders, followed by hematological, metabolic and nervous system disorders. Once hospitalized, the conditions being treated most likely to experiencing drug toxic side effects were quite different, perhaps reflecting the different nature of patients’ medical needs, with cutaneous, general, vascular and cardiac disorders being most affected.
Drugs most likely to produce side effects
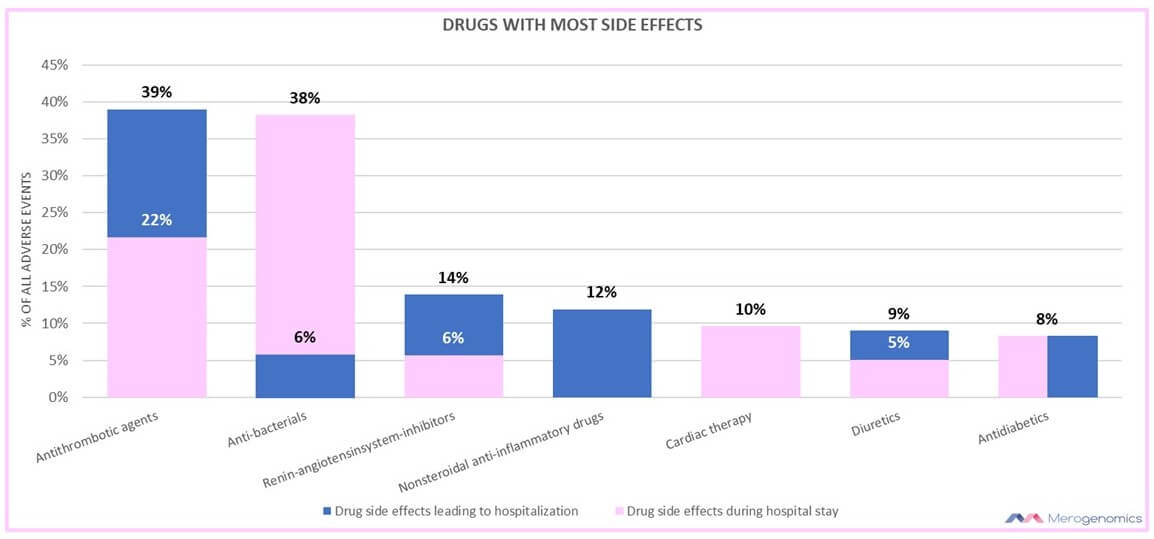
The types of drugs that are most frequently associated with toxic side effects also are a good reason for considering pharmacogenetic testing. Once again, the most affected therapeutic agents are different depending on whether they were medications that led to a hospital admission or were taken during hospitalization.
The most common drug toxic side effect
The most common drug side effects were different between those leading to hospitalization versus those encountered in a hospital setting. Events leading to hospitalization included anemia or bloody stool, most often due to antithrombotics and NSAIDs, followed by hypotension, fainting and acute renal failure (7.7%, 10.3% and 6.1%, respectively), mostly due to RAS-inhibitors.
Events encountered during hospitalization included skin reddening, hypotension, severe skin itching, bloody urine, a reaction at a drug injection site and skin rash. Most of the side effects were due to use of anti-bacterials, with low blood pressure once again mostly due to RAS-inhibitors while bloody urine was linked to antithrombotics.
Most common medical response to drug side effects
Nearly always the suspected drugs were suspended from further use (89.3%), in 8.5% they were continued, and in 2.2% the dosage was reduced.
How are patients affected by drug side effects?
Complete recovery/improvement occurred in most of patients (87.7%), 5.5% had not yet recovered at the time of publication, and 2.9% patients recovered with pathogenic consequences. Fatality was observed 1.0 % of the time. In 2.9% of the cases, the information was not available.
How preventable are drug toxic side effects?
What we really liked about this study (as did the authors of the publication) is that they assessed each adverse drug reaction for the likelihood of being prevented.
| Drugs side effects | Requiring hospital admission | During hospitalization | ||
| Not-preventable/unavoidable | 12.9% | 24.2% | ||
| Probably preventable | 63.9% | 69.4% | ||
| Certainly preventable | 23.2% | 6.4% |
As you can see, a majority of all toxic drug side effects could be prevented with 87% of all such events leading to hospitalization assumed to be preventable, and 76% of all such events in a hospital setting.
This is significant, as each side effect resulted, on average, in an increased 4 days of stay in a hospital. Of those who reported drug side effects, they usually experienced around two different side effects due to medications. Thus there is lots of room to play with in terms of how we can improve medication use in terms of avoiding problematic side effects and it is certain that pharmacogenetic testing could aid in this process.
As the implementation of PGx testing in clinical practice gains ground on a broader level, the ability of prescribing the right drug for the right patient at the right time will be expected to lead to better quality (safer and more effective treatments) and more cost-effective healthcare. The good news is that pharmacogenetic DNA testing is indeed increasing in use, although it is still a very minor component of DNA tests used in clinical practice (less than 5% of ordered DNA tests), with prenatal tests and cancer related tests carving out the lion’s share (approximately three quarters of clinical DNA all testing). Our healthcare systems were not designed for implementing genetics, and as a consequence the healthcare systems are still not prepared to deliver the promise of personalized medicine. But times are clearly changing.
This article has been produced by Merogenomics Inc. and edited by Jason Chouinard, B.Sc. Reproduction and reuse of any portion of this content requires Merogenomics Inc. permission and source acknowledgment. It is your responsibility to obtain additional permissions from the third party owners that might be cited by Merogenomics Inc. Merogenomics Inc. disclaims any responsibility for any use you make of content owned by third parties without their permission.
Products and Services Promoted by Merogenomics Inc.
Select target group for DNA testing
Healthy screening |
Undiagnosed diseases |
Cancer |
Prenatal |
Or select popular DNA test
 |
 |
 |
 |
Pharmaco-genetic gene panel |
Non-invasive prenatal screening |
Cancer predisposition gene panel |
Full genome |